
Improving the effectiveness of medical device donations
September 2022
By Craig Townsend, Director of Healthcare at 42T
Thinking ahead - improving your medical device design for its second life as a donated device
Early in my career, I was offered the opportunity to visit Malawi as part of a commissioned body of work from a global non-governmental organisation (NGO). They wanted to explore how medical device donations could be better managed in territory and what kind of support was needed to make a donation programme effective and viable. The project ended up being cancelled before I ever stepped foot on a plane.
At the time I thought nothing of it. Projects would get cancelled all the time and although I had started to do some research into the ‘problem’, the scale of the issue wasn’t apparent to me. I’m disappointed to say that I stopped thinking about it immediately after being notified that it wasn’t going ahead, missing the point that this project wasn’t meant to be a ‘value add’ and instead was a global call to action.

Access to effective healthcare in low and middle income countries (LMICs) is a big issue and an estimated 4.8 billion people lack safe, timely and affordable surgical and anaesthesia care. This has led to a large number of hospitals, NGOs and medical device companies wanting to support emerging health ecosystems with tools and devices. The easiest way to offer these? Provide LMICs with medical equipment in the form of medical device donations.
Donating? or dumping?
Medical device donations to LMICs should be a positive thing. After all, high-income countries (HICs) donate aid in the form of food, water, clothing and medicine during times of need and these generally promote positive economic empowerment. So why should medical equipment be any different? It’s different, because the devices being donated are not being requested. The vast majority of devices being donated are end of life and deemed no longer suitable for use in HICs. Devices are not being donated - they are being dumped.
Although you would hope that organisations sending ‘old’ equipment have good intentions, the lack of planning and collaboration with LMICs has led to vast amounts of donated equipment being inappropriate, ineffective or even dangerous. The most damning evidence perhaps is that donations are not made by need / demand (it’s not like a hospital in south Sudan requests a haemodialysis machine and receives one). Rather, donations are made by the tonne, often not taking inventory of what is actually being donated. One study even found that 60% of donations were made up of broken equipment.
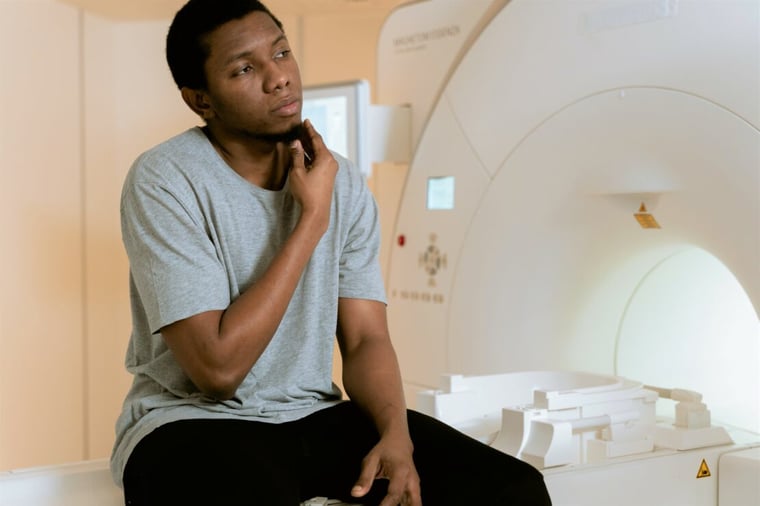
Even where devices work and there is a need, donated equipment may not be appropriate for the LMIC context. Deploying and using a medical device in a country such as Zambia, which has power outages approximately 20% of the year, is completely different to deploying and using it in the United Kingdom. Medical devices are mostly designed for HICs, with reliable infrastructure and trained experts to maintain equipment. In an LMIC, they might simply be unusable.
What’s the problem with a few bits of dodgy equipment?
The justification from HICs is often ‘something is better than nothing’. There are certain economic factors which contribute to the acceptance of ‘dumping’ such as the imbalance between donor and recipient, plus many countries believe it’s culturally inappropriate to decline a gift. An estimated 80% of all medical equipment currently in use in LMICs is equipment which has been donated, so you can see that there is a need. But there are two key problems in donating medical equipment.
Danger to life
If the donated equipment is not working properly / has not been checked prior to being donated, it could be dangerous to use and the recipient may have no knowledge of this danger. Even if the device is working to begin with, recipients may not have access to parts required for servicing, calibration etc. With improper maintenance, the device could develop safety risks down the line.
Danger to the environment
With unsuitable (or broken) equipment being deployed to countries who cannot run or maintain it, it is estimated that 40% of equipment in LMICs is out of use, compared to 1% in HICs. Much ends up in a ‘medical device graveyard’ - essentially a large pile of (potentially contaminated) scrap electronics and metal left to decay. Recycling medical equipment is hard enough in HICs – and can be costly. LMICs often do not have the infrastructure to safely dispose of old equipment, causing a potential ecological disaster.
As a medical device manufacturer, you can help prevent your device entering the graveyard
Improving the suitability of your device for donation at end-of-life is not just the right thing to do. It could help you hit your sustainability or net zero goals, improve brand awareness in rapidly developing healthcare systems, and even add value for the buyer and initial user.
There are a number of ways we in the industry can help tackle the issue of unsafe or unusable devices ending up in LMICs. Whether developing a new device specifically targeted at these markets, or any piece of equipment that could foreseeably be donated later, following a few design principles from repairability to accessibility will help make better, more sustainable products.
Design for sustainability
We can improve the sustainability of a piece of equipment by designing it to last longer. Even if the buyer in a HIC is expected to upgrade the equipment in 3-5 years when a newer model comes along, designing for longevity will mean it can continue to be used once donated. And the original buyer may benefit from reduced breakdowns in its first life.
Related to this is repairability. If a device can be easily disassembled, and repaired using common tools and components, it is more likely that it can go back into service safely. For example, a Philips screwdriver is preferable to a Torx one, or permanent moulded snap features. Following this principle will benefit whoever repairs it in its first life too – whether clinical engineers on site, or the manufacturer’s service team.
Finally, consider the materials and components that will be required during the device lifetime. Ideally, reduce the amount of proprietary single use consumables required (at least for basic functionality) – these may be difficult to source in remote regions. When manufacturing the device itself, use materials such as sheet metal that can be easily sourced in multiple countries. This will increase the chances of a recipient being able to repair a device even if they are unable to import spares, or if they are discontinued.
Design for accessibility
Developing your device to be more accessible will widen the pool of users who can safely use your device – making it more attractive to buyers and safer for those who might receive it as a donation. Aim to make the user interface simple and intuitive to use. And importantly, make the device easy to install and maintain.

Think about how a new user will learn to use and maintain your device. In large products, store user manuals in/on the device – but also upload them for access online. This will enable the device to be used if the manuals are lost, and will enable users to translate them into additional languages using tools such as Google Translate. It's imperfect, but will significantly help those receiving donated devices. Detail or label parts clearly – using multiple languages where required, or clear icons.
Design for the context of use
Across all kinds of medical devices, there is need for products that are appropriate for low-resource settings. For example, electrical equipment that can easily be used in a manual mode during a power outage. Or a device that takes longer to use but does not require imported parts, in a market where labour costs are low and logistics unreliable.
How your ‘LMIC’ device will differ from the ‘HIC version’ will depend on the device type and how it’s used and maintained. To understand the requirements, the design team must get a full picture of this context and different stakeholders’ needs. At 42T, we have developed a variety of devices specifically targeted at LMICs and have learned that shedding preconceptions and engaging with stakeholders in an iterative design process are critical to success.

How can donors better target aid?
Work closely with local health ecosystems
Donation planning is key and both donor and recipient must form an equitable and bilateral partnership. This partnership should lead to the creation of a formal donation plan, which is agreed upon by both in territory clinical and biomedical departments, suppliers, local procurement managers and local health ministers.
Many countries already have national donation policies in place, which can be accessed via government websites, for example The Policy and Procedures Guidelines for Gifts and Donations to the Ministry of Health Jamaica. Countries which do not have a formal, documented donation policy are being supported by organisations such as the World Health Organisation (WHO) and The Tropical Health Education Trust. This has led to the creation of new guidelines such as Medical Device Donations: Considerations for Solicitation and Provision.
These guidelines outline adherence to the WHO principal of ‘good donations’ ensuring maximum benefit for the recipient, whilst respecting their wishes and context, whilst also advising recipients to create lists of prioritised equipment needs including specifications, parts and training needs.
Provide hard cash
The topic of medical device donations to LMICs is becoming better known. There are new studies taking place and guidelines being written attempting to solve the issue, many of which highlight forming closer relationships between donor and recipient as being the key. However, much of this work neglects the topic of financial support.
Access to money ultimately helps solve many of the issues presented by equipment donations, including hiring and training more technicians / engineers, purchasing missing / faulty parts and even purchasing more appropriate equipment outright.
Seek guidance on designing more sustainable, accessible products by speaking with medical device experts
At 42T our world-class engineers, designers and scientists have vast experience in developing simple, intuitive products. We have designed a variety of medical devices specifically targeted at LMICs, considering factors such as minimal training requirements, compatibility with available consumables, and in-country component manufacture.
Our ethnographic research team can help you understand how users from a wide variety of backgrounds and cultures might interact with your device and, crucially, what that means for the design. Our designers can help make your product easier to repair and maintain, either during its initial development or in a redesign for sustainability exercise.
With our knowledge and experience we are the ideal partners to support you in understanding what simple steps could make your device suitable for safe and appropriate donation at end-of-life. The result will be a more sustainable product, a more responsible impact, and of course direct benefit to people’s health worldwide.
Read our healthcare case studies

If you would like to find out more, please contact Craig:
craig.townsend@42T.com | +44 (0)1480 309461 | www.linkedin.com/in/craig-c-townsend
Share this article:
Related Articles

Sustainability, Industrial
EU packaging waste regulations are a significant opportunity

Sustainability, Product Design
The Eco-design Directive for sustainable products - are product owners ready?
Healthcare & Life Sciences
How to rescue medical devices from component problems

What will you ask us today?
We believe in asking the right questions to drive innovation; when we know the right questions, we generate the ideas to answer them.

